Structured medication reviews
NHS England’s structured medication reviews (SMRs) are a NICE-approved, person-centred intervention to optimise medicines use and improve patient outcomes. It involves a comprehensive review of a patient’s medicines and is facilitated through conversations with patients and a shared decision making process.
Prioritising patients for structured medication review
The Network Contract Direct Enhanced Services (DES) requires each Primary Care Network (PCN) to prioritise people who:
- are residents in care homes
- have learning disabilities
- are on complex and problematic polypharmacy, especially those prescribed 10 or more medicines
- are taking medicines associated with medication errors and risk of harm
- are severely frail, isolated, or housebound or who have had recent hospital admissions and/or falls
- are taking potentially addictive medications such as opioids, gabapentinoids, benzodiazepines and Z-drugs.
Priority groups are likely to include patients with multiple long-term conditions or co-morbidities, particularly those with respiratory or cardiovascular diseases, as well as those who have undergone a comprehensive geriatric assessment.
Additionally, other patients may need to be reactively referred for SMRs based on specific clinical needs or concerns.
Inviting patients for a structured medication review
Once a patient is identified for an SMR, invite them with a clear explanation of the process. Clearly outline that the review involves a shared decision-making conversation to assess their medications, ensure they remain effective and are still appropriate for their needs. Encourage them to bring their medications to the appointment and prepare any questions or concerns they want to discuss.
The Health Innovation Network’s resources to support patients having an SMR are available in various community languages.
Structured medication review framework
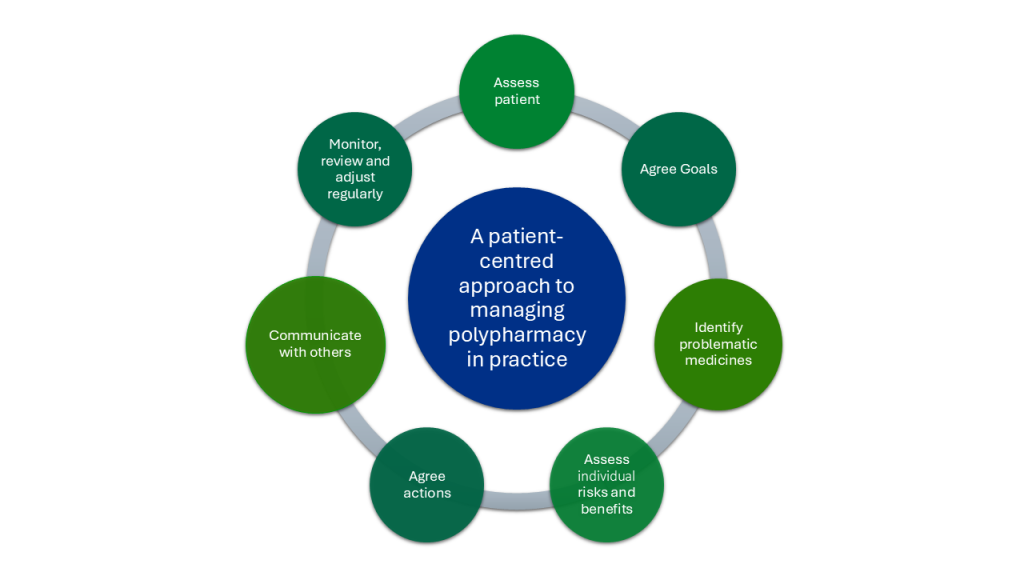
The SMR framework ensures that a patient’s medicines are both effective and aligned with their individual needs. By adopting a person-centred approach, it aims to reduce inappropriate polypharmacy while prioritising the individual’s health goals and preferences. The framework follows a seven-step process, adapted from established polypharmacy, multimorbidity and frailty guidelines (available from BMJ):
Update history
- Further information section removed, as information available elsewhere in article. Three-talk model link updated. Minor formatting updates.
- Added 7 steps of polypharmacy infographic.
- Republished
- Full review and update of article. Originally published 12th January 2022.
- Published